If I could hop in a time machine and travel back to when I first received my diagnosis and started CPAP therapy, there are so many pieces of advice I wish I could give my younger self. Until time travel becomes a reality, I hope that by sharing 6 things I wish I had known starting out with CPAP you can avoid some of the pitfalls and curveballs I dealt with early on. I’m Emma Cooksey, and I’m a real-life sleep apnea patient.
1. Women Have Sleep Apnea Too
When I received my diagnosis with obstructive sleep apnea (OSA) in 2008, I believed the stereotype that only older, overweight men had sleep apnea. This was reinforced when I unpacked my CPAP machine, because I saw pictures of elderly men in the instruction manual. I felt shame and embarrassment to be a young, healthy woman with this condition.
Thankfully, things are beginning to change, and healthcare professionals (like those at Aeroflow Sleep) are becoming more used to seeing people of all genders, backgrounds, and body types being diagnosed with obstructive sleep apnea.
I wish I could go back to my younger self around the time I was diagnosed and reassure myself that anyone–-including women—can have sleep apnea. Rather than hiding and feeling embarrassment about my CPAP, I would have framed it as a treatment! After all, I deserve to feel better and avoid future serious health consequences.
2. Adapting To CPAP Therapy Takes Time
The first few nights I spent with my CPAP were terrible. I struggled to keep my ill-fitting mask on my face longer than 10 minutes at a time. Knowing that some people take time to adapt to CPAP therapy would have helped me. Instead of panicking that things weren’t going well, I could have focused on the progress I was making night to night.
Over the first few weeks, I gradually went longer and longer stretches wearing my CPAP. I wish I could go back and celebrate the wins of improving my CPAP use gradually, rather than feeling like I was failing, because I couldn’t use it the whole night those first few weeks.
This isn’t always the case for everyone, but it seems to be more common than not. And if you don’t see any improvement, that’s okay! Speak up! Ask your doctor or dedicated Aeroflow Sleep Specialist about other options. You may need to adjust that ill-fitting mask (like I did,) try different pressure settings, even look into CPAP alternatives.
3. Finding The Right Mask Fit Is Everything
When I was first handed my CPAP machine all those years ago, the DME employee gave me a full-face CPAP mask, size Large. I had never tried on a mask before and didn’t know anything about how they should fit my face. Once more, if I could go back in time, I would tell myself that loud whooshing noises coming from escaping air at the side of my mask are a sign that the mask doesn’t fit properly.
I learned the hard way that there are multiple manufacturers, and each has masks that fit slightly differently. I struggled with my first mask, because my size is actually Medium. I can only imagine how much more quickly I could have adapted to CPAP therapy if I had found the correct mask the first week rather than months and months later. What’s more, had I been given the wrong type of CPAP mask, the struggle may have put me off using CPAP altogether.
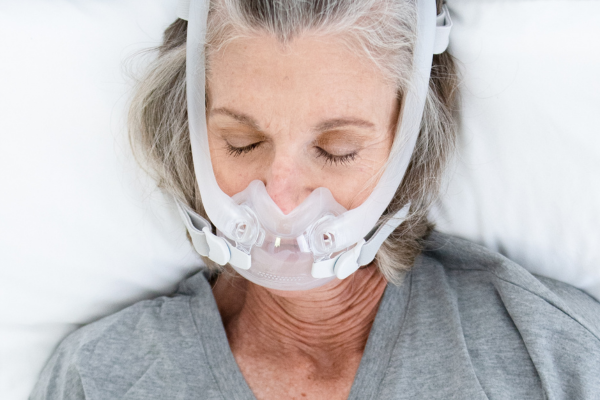

There are 3 traditional types of CPAP masks: full-face, nasal, and nasal pillows masks. Aeroflow Sleep carries all of them, plus a hybrid model called Bleep that doesn’t need headgear. More importantly, they offer a revolutionary mask-fitting technology. By answering a few questions and submitting a selfie, this amazing innovation tells you exactly what make, model, and size CPAP mask is recommended for your unique face shape. I absolutely would’ve switched CPAP suppliers just to try that service all those years ago!
4. Comfort Can Make All The Difference
Your mask isn’t the only thing that can provide extra comfort to your CPAP. I’m always astonished when I ask a patient about their comfort settings and they say, “What are those?” Or, some think, “You mean my pressure setting?” A pressure setting is the airflow level(s) prescribed by your doctor to keep your airway open at night. There are also CPAP comfort settings, which not only can be changed by the CPAP user but should be changed to maximize comfort. For example, Resmed calls their Expiratory Pressure Relief (EPR.)
Different parts can help make your CPAP therapy more comfortable, too. My first CPAP machine was pretty basic. I hadn’t even heard of a humidifier, and it was only once I visited online forums with other CPAP users that I realized I could buy a humidifier, which would solve my dry mouth problems. Today’s machines often have a humidifier integrated in their design. Make sure yours does, because humidification level can be turned up and down depending on your own preference and make a huge difference.
Temperature can also be controlled if you purchase a heated element; like heated humidifiers or heated tubing. Both can be controlled in comfort settings. It took me a while to learn that my rainout—where condensation gathers in CPAP tubing—could be prevented with a heated hose. This does not come standard with most machines though and is not typically covered by insurance; be prepared to pay out-of-pocket for them. Still, starting out, it would have been great to have this information upfront to avoid so much trial and error to alleviate rainout.
5. Social Support Really Helps
Remember when I mentioned forums? Well, I felt isolated and alone for years with my sleep apnea diagnosis and CPAP therapy until I found those. Some of my closest friends didn’t know that I dealt with sleep apnea or used a CPAP. Finding social support is invaluable. Sure, I never found Facebook groups or online forums to be my cup of tea before, but there are many different groups offering advice and connection. Many larger cities actually have physical meetup groups to support people with sleep apnea. Check what’s available in your area!
Nonprofits, raising awareness about sleep apnea or sleep disorders in general, can be great ways to connect with other sleepyheads, nurturing your sleep apnea journey for positive change. Most charities and nonprofits have a social media presence, too, if that’s your thing, and events throughout the year to take part in. I, myself, have a podcast called “Sleep Apnea Stories” where you can continue to hear about my own sleep apnea learnings.


Simply knowing there are other patients with similar journeys to my own has transformed my experience of living with sleep apnea. I no longer feel isolated and alone and have made some great friends and connections along the way. I definitely wish I had been told about social support as a key element of living with a sleep disorder when I was first handed my CPAP.
6. Sleep Apnea Changes Over Time
Last but not least, sleep apnea changes over time. When my kids were little, I didn’t always keep my annual appointment with my Sleep Specialist. Life got busy and I was much more likely to follow up on my kids’ health than my own. I wish I had known then what I know now; sleep apnea is a chronic condition that fluctuates with your age, weight, mental health, etc. It’s super important to visit your doctor regularly so that you can discuss any changes in symptoms that might require an adjustment to your CPAP pressure. It took me feeling much worse [again] to realize, I needed to go and see my Sleep Specialist and have my CPAP adjusted.
I have been a CPAP user for more than a decade now, and most of that time has been smooth sailing. Those first few months had some rocky ups and downs, which I know now could have been alleviated with the right advice and support. I highly recommend Aeroflow Sleep for their resources and guides. It’s clear that they care about their patients, because obviously, they have me to tell you all about this stuff (ha!) In conclusion, I hope these pointers help you to adapt to therapy quickly and resolve any issues before feeling the diagnosis is insurmountable.