Apnea-Hypopnea Index is not the easiest thing to say five times fast. It’s also not a widely discussed scale of measurement until you’re faced with a sleep disorder. This makes it rather intimidating for anyone newly diagnosed with sleep apnea. You’re probably wondering, what does the Apnea-Hypopnea Index quantify? Can I improve my AHI score? Am I going to die? Aeroflow Sleep is here with the answers and more.
What Is AHI?
Rest easy; AHI is not like stages of cancer, so don’t think you’re at death’s door if yours is higher than others. AHI is simply the number of apneas and hypopneas you experience within an hour of sleep over your total sleep time.
An apnea is when you stop breathing during sleep. If an apnea event occurs, it’s a potential sign of obstructive sleep apnea (OSA) and requires continuous positive airway pressure (CPAP;) OSA’s tried and true treatment option. An apnea can also be a sign of central sleep apnea (CSA,) which is a neurological disorder and still can be treated with CPAP, but OSA is most common.


Hypopneas are intervals of shallow breathing, and moderate to severe hypopneas can cause health problems without CPAP therapy prescribed. A combination of both apneas and hypopneas would absolutely require CPAP, especially if your AHI score exceeded a certain threshold.
How Is AHI Calculated?
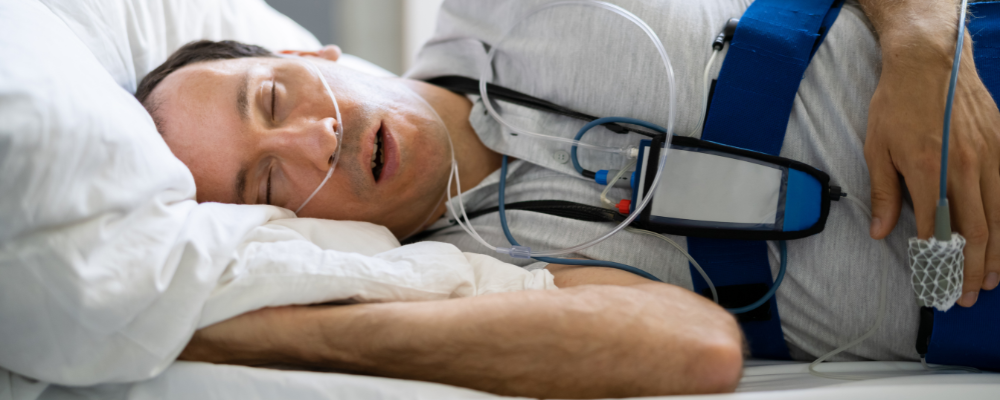
If you think you have sleep apnea or your partner notices apnea events while you sleep, tell your doctor. They will likely order an overnight sleep study, either in-home or in a lab. A few non-invasive sensors will monitor your breathing pattern, airflow, oxygen levels, and heart rate to determine the cause of your sleep problems. Most importantly, the data collected will be used to calculate your AHI or severity of sleep apnea.
Insider Tip: Other symptoms of sleep apnea may include daytime sleepiness, insomnia, headaches, mood swings, and snoring. Ask your doctor if a sleep study is right for you.
What Is a Normal AHI Score?
The cutoff for an ideal AHI is 5. That means a normal AHI score is anything below 5 for an adult, but an AHI of 1 or more is enough to diagnose a child with OSA. If you are at least 18 years old and have an AHI above 5, you would then fall into one of 3 sleep apnea categories:
- Mild Sleep Apnea: An AHI ranging between 5-15
- Moderate Sleep Apnea: An AHI ranging between 15-30
- Severe Sleep Apnea: An AHI of 30 or more
Again, these categories do not come with a mortality rate, but your doctor needs to know what your particular condition is in order to prescribe the right treatment for you.
Treatment is more than likely going to make you a CPAP user. OSA patients use CPAP machines to regulate their breathing while sleeping, and positive airway pressure (PAP) levels positively affect your AHI. For example, a patient with severe OSA will probably be prescribed a higher air pressure than someone with only 6 apnea events per hour, because obstructive apneas are more difficult to bypass.
Not all CPAP machines have a set PAP level though. Auto-titrating CPAP machines are smart and adjust the air pressure depending on where you are in your sleep cycle. Pressure is a constant flow while inhaling and exhaling, so ask your doctor what range best suits you. After all, it’s necessary to manage your AHI once you’ve comfortably drifted into REM sleep.


What Does My AHI Mean For My Treatment?
An auto-titrating device–like the ResMed AirSense 10 AutoSet–uses a ramp function to literally “ramp up” to its set pressure over time, as you fall asleep. You can also adjust your pressure as needed with the help of a doctor.
Regardless, research tells us that using a CPAP machine can decrease your AHI by 73%, plus we know 3 additional ways you can lower your AHI tonight.
How Do I Lower My AHI?
Although you can lower your AHI, it’s possible for it to increase too. Some reasons are within your control including those we discussed; like alcohol use, sleeping position, and weight gain. Others may be a little more complicated.
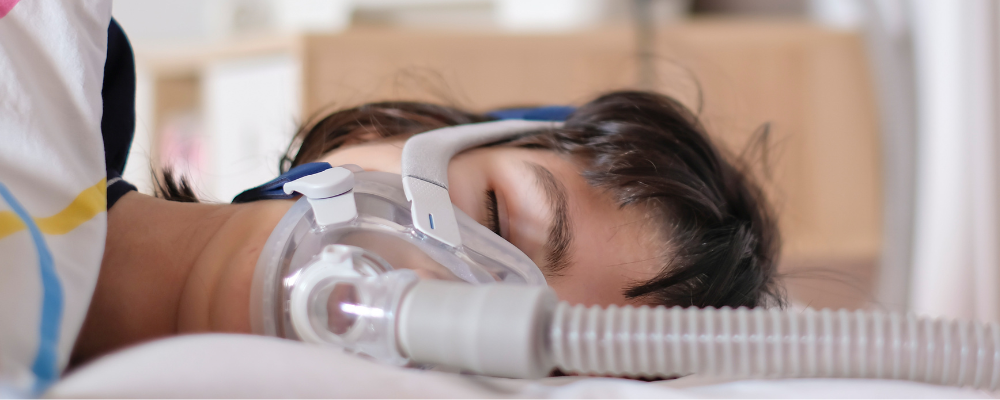
The CPAP mask you wear is often as important as using the CPAP machine itself, because a mask leak can cause your AHI to increase. A mask leak can occur a few different ways. If you feel air blowing in your face, all you may need to do is adjust your mask straps; Michelle can show you how.
If an adjustment doesn’t fix your mask leak, it’s possible that your CPAP mask is not right for your face shape. Luckily, a new AI mask-fitting technology is available to all members of the Aeroflow Sleep program, both newly diagnosed and existing patients. All you need to do is ask your dedicated Aeroflow Sleep Specialist to send the link to your smartphone.
A realistic AHI depends on risk factors and preexisting comorbidities; including hypertension, cardiovascular disease, and obesity. Once you’ve determined your AHI with a sleep study, you can then use that information to set baseline goals with your doctor. Some of Aeroflow Sleep’s licensed healthcare professionals recommend the 3 following ways you can lower your AHI tonight:
1. Avoid Alcohol
One alcoholic beverage every now and then isn’t enough to upset the balance of your AHI. If you like to imbibe more than once a week though, it’s time to cut back.
According to the American Journal of Managed Care, alcohol consumption contributes to lower oxygen saturation (or blood oxygen levels,) especially among those who snore and have OSA. That means that patients with an increased risk of OSA are worsening their ability to breathe with every drop.
Michelle Worley, Aeroflow Sleep’s Director of Clinical Operations has more to say about your nightcap here.
2. Change Your Body Position
Next, if you are a stomach or back sleeper, you may want to try sleeping on your side instead. Changing your body position isn’t easy, but it will dramatically improve your quality of sleep and quality of life.
To go from sleeping on your back or stomach to sleeping on your side, try purchasing a body pillow and fit it against your new body position at night. You may experience a little neck and shoulder pain in the early stages, but it doesn’t matter if you try sleeping on your left or right side. It all depends on what’s more comfortable for you.
Michelle adds, “Sleeping on your side with your head slightly elevated is best for breathing problems. In fact, sleeping with the head of your bed elevated will help reduce gastroesophageal reflux, commonly known as acid reflux or gerd, and heartburn symptoms.” It may also help people with high blood pressure and neck pain.
3. Eat Right & Exercise Regularly
Finally, significant lifestyle changes all circle back to diet and exercise. Generally, sleep apnea symptoms like daytime sleepiness and comorbidities like cardiovascular disease and excess weight can be treated thus. For example, daytime sleepiness can be curbed with a cup of coffee. Patients with heart disease should avoid fatty foods. And excess weight can be shed with regular exercise.
Perhaps talking to a nutritionist–like Dr. Monique May, Board-Certified Family Physician and partner of Aeroflow–can help, in addition to your primary care doctor and Aeroflow Sleep Specialist. In fact, Dr. May has an entire list of foods you need to eat and avoid if you have sleep apnea.
What Causes AHI To Increase?
Once you’ve clicked on the link, you’ll be asked a series of questions and to take a selfie, then voila! Watch the algorithm work to find your perfect fit!
Finally, taking new medications, particularly sedatives can cause your AHI to increase. Even melatonin has negative effects on persons with OSA. Dr. May says it may “cause the muscles of the throat and upper airway to relax too much, worsening the obstruction seen with sleep apnea.” Drug interactions are also possible with blood thinners, diabetic supplements, and antidepressants. Talk to your doctor before starting any type of over-the-counter or prescribed medicines while being treated for sleep apnea.
Talk To Your Doctor About Aeroflow Sleep
A lot of ongoing doctor interaction is likely to occur when you’re on CPAP, which is why Aeroflow Sleep is here to take care of everything for you. In fact, we specialize in getting your CPAP equipment covered up to 100% through insurance; primary, secondary, Medicare, and Medicaid.
We also understand that navigating the insurance process can be overwhelming. If understanding your AHI wasn’t difficult enough, terms like deductible and coinsurance are very confusing. We’ll answer any questions you may have along the way, especially medical ones.
Our US-based call center is standing by with clinicians and dedicated Sleep Specialists ready to assist you. So, talk to your doctor about Aeroflow Sleep, America’s #1 fastest-growing CPAP equipment provider today.