Have you ever Googled “sleep apnea?” Maybe you’re an avid WebMD-er, or maybe you’re just curious about what sleep apnea even is.
When you do a quick search on sleep apnea, you will quickly learn that it is a sleep disorder that impacts your breathing while sleeping. Wikipedia says, “Sleep apnea is a result of ‘pauses in breathing’ or ‘periods of shallow breathing during sleep,’” but what exactly does this mean?
Don’t worry; Aeroflow Sleep is about to get into the nitty gritty of all things “pauses in breathing” and “shallow breathing” below. So, take a deep breath—see what we did there—and let’s dive in!
What Do Pauses In Breathing Mean?
As the phrase suggests, a pause in breathing means that your breathing stops or slows for a period of time. According to MedlinePlus.gov, a pause in breathing is medically referred to as an “apnea.” These pauses can look and feel different depending on your situation, and they can occur both while you’re asleep or awake. When you’re asleep, you’re unlikely to remember experiencing an apnea. However, when you’re awake, this phenomenon is quite noticeable.
Here are a few examples of irregular breathing patterns that can occur when you’re awake as a result of pauses in normal breathing:
- Bradypnea: This is the result of an extremely low breathing rate, and it is typically accompanied by dizziness, fatigue, and confusion due to low oxygen levels. And, according to Healthline, it can be caused by hypothyroidism, head injury, or opioid use.
- Dyspnea: More commonly known as “shortness of breath,” dyspnea is the sensation where you feel like you can’t get enough air, and the Cleveland Clinic notes, it’s often a result of heart or lung conditions; like heart failure or pneumonia.
- Cheyne-Stokes Breathing: Finally, according to the National Library of Medicine, this is “a [standalone] breathing disorder that causes episodes of apnea and hyperventilation.” It often accompanies heart failure and stroke, and interestingly enough, was first studied in 1876 by French physician, Camille Biot.
That’s a lot of scientific jargon, we know, but if you are experiencing any irregularity in breathing during the daytime or nighttime, it is urgent for you to reach out to your doctor. If left untreated, an apnea—regardless of severity—can lead to an increased risk of hypertension, heart disease, and diabetes.
What Does Shallow Breathing Mean?
Shallow breathing is the opposite of a calming, deep breath; it is short inhales and exhales that do not fill the lungs up with their full capacity of air. Unfortunately, this means shallow breathing can put a lot of stress on the body and lead to an elevated heart rate and blood pressure.
Paraphrasing what the National Heart, Lung, and Blood Institute says, our breathing is controlled by our autonomic nervous system, meaning that we don’t have to consciously think about breathing. However, a physical blockage of your airway, and/or a lack of signals sent to your brain stem, can cause shallow breathing. Episodes of shallow breathing are called ‘hypopneas’ and can be classified based on what their cause is.
Do Both Point To Sleep Apnea?
Yes, both pauses in breathing (apneas) and shallow breathing (hypopneas) are key warning signs that may point to sleep apnea when they occur during sleep. However, because these apneas and hypopneas happen while you’re sleeping, you might not be aware they’re happening.
You may notice other symptoms; such as loud snoring, daytime sleepiness, weight gain, gasping during the night, and irritability. It’s important to note that these symptoms are not a “one size fits all;” sleep apnea symptoms may present differently depending on the person. So, ask your bed partner if they notice symptoms while you sleep, and be cognizant of what you’re feeling when you wake.
Not only do symptoms vary, the type of sleep apnea that you’re diagnosed with can, too. There are 3 different types of sleep apnea: obstructive sleep apnea, central sleep apnea, and mixed sleep apnea. Obstructive sleep apnea (OSA) happens when your upper airway is physically blocked while sleeping, which causes breathing to stop for a period of time. Central sleep apnea (CSA) is a result of the brain not sending signals to the body to breathe while sleeping. Mixed sleep apnea is a combination of the two.


But, why should you care? Well, sleep apnea is a serious medical condition that can lead to other health-related issues; such as stroke or heart attack. Sleep apnea puts a lot of strain and stress on the body, and it’s imperative that you get a good night’s rest for your overall health, regardless of whether you have sleep apnea or not.
What Should I Do If I Have Sleep Apnea?
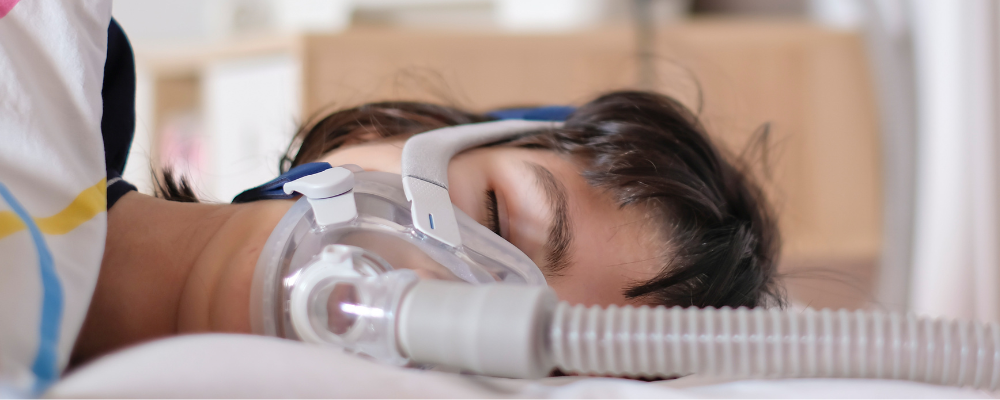
The American Academy of Sleep Medicine recommends continuous positive airway pressure (CPAP) as the treatment option for all 3 types of sleep apnea. If you think you or a loved one may have sleep apnea, reach out to your healthcare provider.
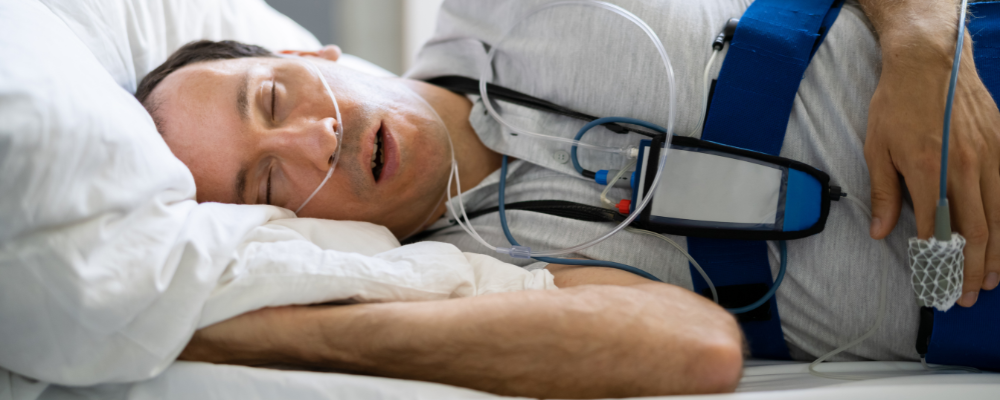
Your doctor can take your symptoms into account and recommend completing a polysomnography, or sleep study, either in-lab or at home. If your sleep study reveals that you have sleep apnea, they will likely write a prescription for your new PAP device; be it an APAP, BiPAP, or CPAP machine.
Aeroflow Sleep is here to help you order yours (and any supplies you need) through insurance. By filling out our online qualifying form below, we will verify if your insurance is in-network with us. After all, good sleep matters!
If you’ve been diagnosed with sleep apnea, get started with Aeroflow Sleep today:
References
“Sleep Apnea.” Wikipedia, Wikimedia Foundation, 30 Oct. 2023, en.wikipedia.org/wiki/Sleep_apnea.
“Breathing - Slowed or Stopped: Medlineplus Medical Encyclopedia.” MedlinePlus, U.S. National Library of Medicine, 2 Feb. 2023, medlineplus.gov/ency/article/
003069.htm.
“Bradypnea.” Cleveland Clinic, Cleveland Clinic, 17 Mar. 2023, my.clevelandclinic.org/health/symptoms/24832-bradypnea.
Pietrangelo, Ann. “Bradypnea: Causes, Symptoms, and Treatment.” Edited by Judith Marcin, Healthline, Healthline Media, 24 Apr. 2023, www.healthline.com/health/
bradypnea#causes.
“Dyspnea (Shortness of Breath): Causes, Symptoms & Treatment.” Cleveland Clinic, Cleveland Clinic, 11 Nov. 2022, my.clevelandclinic.org/health/symptoms/
16942-dyspnea.
Rudrappa, Mohan, et al. “Cheyne Stokes Respirations.” National Library of Medicine, StatPearls, 31 July 2023, www.ncbi.nlm.nih.gov/books/NBK448165/.
“The Breathing Pause.” ATS Quick Hits, American Thoracic Society, www.thoracic.org/professionals/clinical-resources/quick-hits/the-breathing-pause.php. Accessed 2 Nov. 2023.
Rifkin, Rachael. “How Shallow Breathing Affects Your Whole Body.” Headspace, Headspace, 13 Oct. 2023, www.headspace.com/articles/shallow
-breathing-whole-body.
“How Your Body Controls Breathing.” National Heart Lung and Blood Institute, U.S. Department of Health and Human Services, 24 Mar. 2022, www.nhlbi.nih.gov
/health/lungs/body-controls-breathing.
Summer, Jay. “What Is Hypopnea?” Edited by Abhinav Singh, Sleep Foundation, Sleep Doctor Holdings, 24 Oct. 2023, www.sleepfoundation.org/sleep-apnea/
hypopnea#references-78244.
“American Academy of Sleep Medicine Guidelines: AASM.” American Academy of Sleep Medicine – Association for Sleep Clinicians and Researchers, American Academy of Sleep Medicine, 28 Sept. 2023, aasm.org/clinical-resources/practice-standards/practice-guidelines/.