In 2019, ResMed published an article with the title: More Than 936 Million Have Obstructive Sleep Apnea [OSA] Worldwide. It was a figure – backed by research found in Lancet Respiratory Medicine’s literature review – that provoked physicians to “step up their efforts.” After all, the new data suggested the World Health Organization (WHO) was off by a number nearly 10 times greater than its estimate of 100 million people.
Fast-forward to 2022, and ResMed has not edited its publication, nor changed its stance on the threat we face if the prevalence of sleep apnea goes unchecked. It’s probable that sleep apnea estimates top 1 billion people now! That’s why today’s blog is going back to the basics. We’ll answer general questions like what is sleep apnea, what are its symptoms, how to know if you have it, and more. Aeroflow Sleep is here to help you educate yourself.
What Is Sleep Apnea?
Sleep apnea is a breathing disorder that occurs while you are sleeping. Episodes when you stop breathing are called apneas, and each time you stop breathing prevents oxygen from reaching the brain. This can happen for a variety of reasons, yet each reason is associated with a specific sleep apnea type.
Obstructive Sleep Apnea (OSA) is when your airway is literally obstructed by something; such as a fatty neck, enlarged tonsils or adenoids, or simply your throat muscles relaxing to the point that they collapse. Because so many factors fall into this category, it is the most common type of sleep apnea.
Central Sleep Apnea (CSA) only happens when your brain is failing to function properly. Signals are sent to the brain along the central nervous system, and some signals tell it how to breathe. When these signals are broken, you stop breathing, and when it occurs during sleep, you get CSA.
Mixed Sleep Apnea is also known as Complex Sleep Apnea or Treatment-Emergent Central Sleep Apnea. Regardless of what you choose to call it, this sleep apnea type is reserved for the unfortunate few who have both OSA and CSA. It is also the most severe.
What Are Sleep Apnea Symptoms?
To make matters worse, your body will often attempt to compensate for your sleep apnea, which may present itself as symptoms. If you have OSA, collapsed muscles often cause loud snoring, because the tissues are now vibrating against one another every time a breath tries to bypass the blockage. Or, you may breathe through your mouth instead, hoping to achieve more airflow, but then you suffer from a dry mouth or sore throat in the morning.
Here’s a list of symptoms–excluding those previously mentioned–that may indicate you have untreated sleep apnea:
- Excessive daytime fatigue
- High blood pressure
- Gasping or choking at night
- Morning headaches
- Irritability or mood swings
- Insomnia
- Weight gain
How Do You Know if You Have Sleep Apnea?
Did any of those symptoms sound familiar to you? It’s even more likely that you have sleep apnea when you have symptoms as well as certain pre-existing conditions. Obesity, type 2 diabetes, heart disease, hypertension, or a family history of these comorbidities put you at a higher risk for sleep apnea.
You may also fit the sleep apnea stereotype, which is often portrayed as an elderly, overweight white male. However, it’s important to note that you can still have sleep apnea if you’re young, skinny, a woman of color, or even suffer zero chronic health problems. And besides, the National Institutes of Health (NIH) states, “22 million Americans have sleep apnea, and 80% don’t know it.” They can’t all be elderly, overweight white males.
The only way to know for sure is to ask your doctor about a sleep study.


How Do You Treat Sleep Apnea?
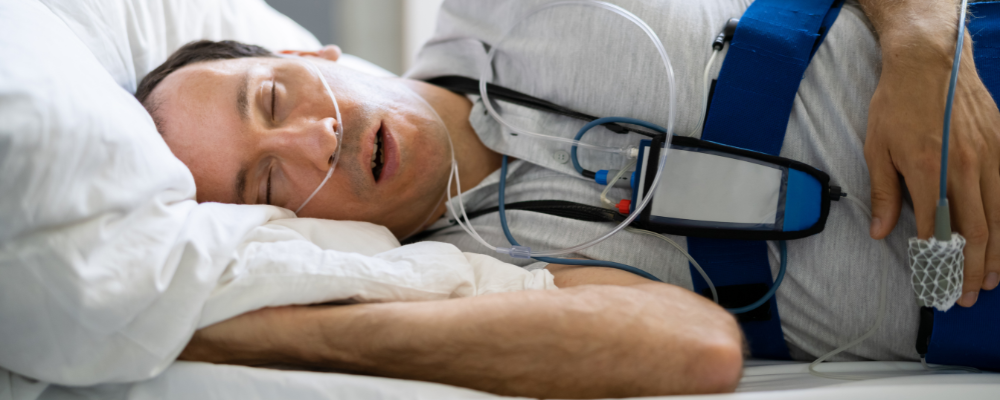
In order to treat your sleep apnea, you first have to know you have it. A sleep study is performed overnight, either in a lab or at home, and will assess your breathing pattern, airflow, oxygen levels, and heart rate while you sleep. If you stop breathing more than 5 times per hour during your sleep test, congratulations! You have sleep apnea.
How you treat sleep apnea is up to you. The Mayo Clinic suggests everything from lifestyle changes to oral appliances to surgery. Aeroflow Sleep recommends continuous positive airway pressure (CPAP) therapy, which the Mayo Clinic agrees is “the most common and reliable method of treating sleep apnea.”
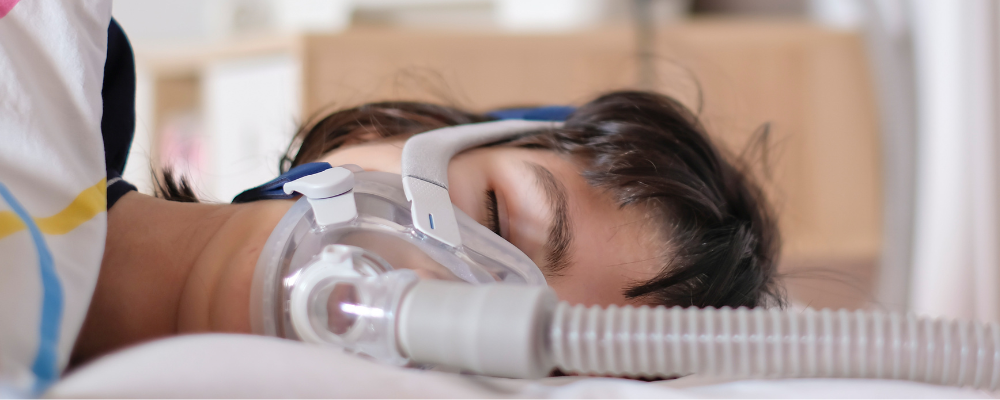
CPAP therapy is when you use a CPAP, BiPAP, or APAP machine to deliver a constant stream of airflow through a CPAP mask and into your breathing passages; such as your nose, mouth, or both. That stream of air prevents your throat muscles from collapsing and compensates for any malfunctioning brain signals all in one CPAP device.
Special CPAP supplies and accessories can even alleviate some of the symptoms we mentioned earlier. For example, attaching heated tubing and a humidifier keeps the air warm and moist, so you’ll wake up feeling refreshed; not fighting a dry mouth or sore throat. The best part is that many of these products are covered by insurance.
Is CPAP Covered by Insurance?
Yes, CPAP equipment is covered by insurance! Aeroflow Sleep works directly with your insurance provider to ensure you get the best possible coverage available to you without the hassle of figuring out the process alone. Many private insurance plans are accepted; including Aetna, Blue Cross and Blue Shield (BCBS,) Cigna, Humana, and United Healthcare. We also take most Medicare and Medicaid programs.
To get started and see what your estimated cost might be, fill out a simple form to determine if your insurance plan is eligible for CPAP from Aeroflow Sleep. Then, tell us which CPAP supplies you currently use. If you’ve never tried CPAP before, have your doctor give us a call! We will work with them to submit all required paperwork – a recent sleep study and prescription – to your insurance provider. It’s as simple as that.
We ship all orders right to your door in discreet packaging and notify you both when it’s time to replace your parts and when the manufacturer releases an update. So, don’t feel stuck being one in a billion. Aeroflow Sleep will fully support you on your sleep apnea journey and simplify your life as you navigate a new (or existing) diagnosis.
References
Benjafield et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respiratory Medicine 2019. http://dx.doi.org/10.1016/S2213-2600(19)30198-5
Lee, Won, et al. “Epidemiology of Obstructive Sleep Apnea: a Population-Based Perspective.” National Library of Medicine, National Center for Biotechnology Information, 7 Aug. 2009, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2727690/.
Staff, Mayo Clinic. “Sleep Apnea.” Mayo Clinic, Mayo Clinic, https://www.mayoclinic.org/diseases-conditions/sleep-apnea/diagnosis-treatment/drc-20377636.
Information provided in blogs should not be used as a substitute for medical care or consultation.