I, Emma Cooksey, may have gone undiagnosed with obstructive sleep apnea (OSA) for 10 years, but there was no way a doctor could miss my depression. I distinctly remember sitting in a drab doctor’s office on a rainy Tuesday morning with tears streaming down my face, noisily blowing my nose and struggling to be understood between sobs. I was 23 and had recently switched jobs. I felt overwhelmed, sad, and hopeless, but I came out on the other side. You can, too, and my story is just one way it was possible.
Where OSA Was Overlooked, Depression Flourished
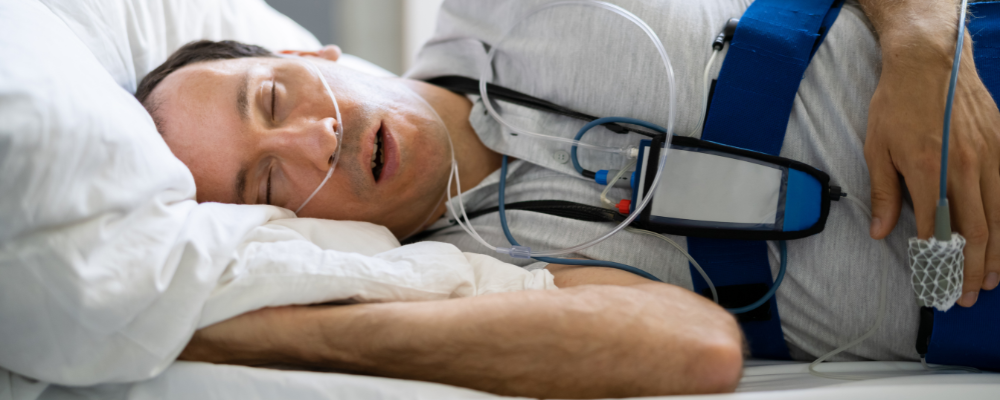
I remember outlining some symptoms, which I know now (with hindsight) indicated OSA, could be a factor. Those symptoms included daytime sleepiness, waking up gasping, and morning headaches. However, I can see now from the doctors’ perspective that those were easy to miss when I showed up crying.
I described how miserable I had been feeling. I described struggling to get out of bed and no longer taking much pleasure from activities I used to enjoy. And, I explained the debilitating anxiety, which showed up as constant worry about future events and outcomes. After listening intently, the doctor explained she thought I was dealing with depression and anxiety.
She prescribed an antidepressant and referred me for Cognitive Behavior Therapy (CBT) with a professional counselor. Of course, I was open to whatever my doctor thought would help, because I’d been feeling so bad; I was willing to try anything to feel better. Unfortunately, I didn’t immediately feel better.
It took around 3 months before I started to really see an improvement in my mood, and I still had undiagnosed obstructive sleep apnea.
Can Treating Depression Help OSA?
When I consistently took antidepressants and completed the CBT exercises, I found my feelings of apathy receded, and I was able to experience life again without the cloud of depression weighing on me all the time. Yet, waking up in the morning was still a struggle for me; it was not inherently treating my OSA, and research tells us that the severity of obstructive sleep apnea will not subside more than 15% with therapy but without a CPAP machine.
Now, I have found my depression and anxiety ebbs and flows with different life stages. After the birth of my first child, I experienced a resurgence of my depression symptoms. Postpartum depression is common and much more understood now than it was for generations of women who came before. In fact, postpartum depression can exacerbate OSA, and I was still undiagnosed at the time.


It was being surrounded by my friends and family who could see I was struggling that encouraged me to see my primary care physician. Upon the suggestion of my physician, I started therapy with a licensed mental health counselor for some extra support; not CPAP therapy.
At first, I wasn’t sure showing up to an office and spilling my guts to a stranger would help. However, very quickly, I started to feel a lot better again. I wasn’t so overwhelmed, and I had tools to fall back on when the bad days inevitably came. That is where I began to see the connection between my sleep issues and my depression.
The Light At The End Of A Very Dark Tunnel
One recurrent thought that bothered me was the idea that I was the only one struggling. I explained to my therapist, “Everyone else seemed to be dealing with life without bursting into tears all the time!”
At this remark, my therapist chuckled and swung her computer screen around. I couldn’t make out the writing, but I could see that it was a calendar, completely full. “Do you see all these colored boxes? Those represent all the appointments I have this week with women just like you struggling with anxiety and depression. Plus, I have a long waitlist,” she exclaimed!
My therapist’s professional experience is reflected in surveys conducted by the National Institute of Mental Health. She even aided in research that shows, “An estimated 21.0 million adults in the United States have at least one major depressive episode. This number represents 8.3% of all U.S. adults. The prevalence of major depressive episodes was higher among adult females (10.3%) compared to males (6.2%).”
I am far from being alone in my struggles, and I began to realize that I was in good company. My therapist became my light at the end of a very dark tunnel. I started to see my mental health as something I had some agency in where I hadn’t previously, and—little did I know—my newfound empowerment put me on the path to succeed in my sleep apnea treatment.
Why Diet & Exercise Really Matters
I read a few articles about how powerful exercise can be for people with depression. Even though going to a gym never appealed to me, I began walking every day and, as it became a habit, I noticed an improvement in my mood.
Don’t just take my word for it; the research into exercise and depression agrees. The British Medical Journal, or BMJ, published, “Some interventions with few costs, side effects, or pragmatic barriers, such as walking and jogging, are effective across people with different personal characteristics, severity of depression, and comorbidities.”
Another change I made more recently was giving up alcohol. Growing up in Scotland, drinking alcohol is very much part of the culture. Socializing in pubs is a favorite national pastime, and I never considered myself as having a problem with alcohol; nothing like alcoholics who need to maintain sobriety to keep their life on track. However, reading Quit Like a Woman: The Radical Choice to Not Drink in a Culture Obsessed with Alcohol by Holly Whitaker gave me a brand new perspective. This quote particularly spoke to me:
“If you drink one glass of wine, you might have about twenty minutes of the desired ‘relaxed’ effect before the drug wears off, and you’re left with increased amounts of cortisol and adrenaline, which fuel anxiety. This means alcohol causes anxiety; it doesn’t manage it.”
When I stopped drinking three years ago, I didn’t know whether I would continue my sobriety. What started as a one-month break turned into a lifestyle change with which I do intend to continue, and the main difference I noticed was improved sleep.
Set Psychological Precedence With Your Doctor
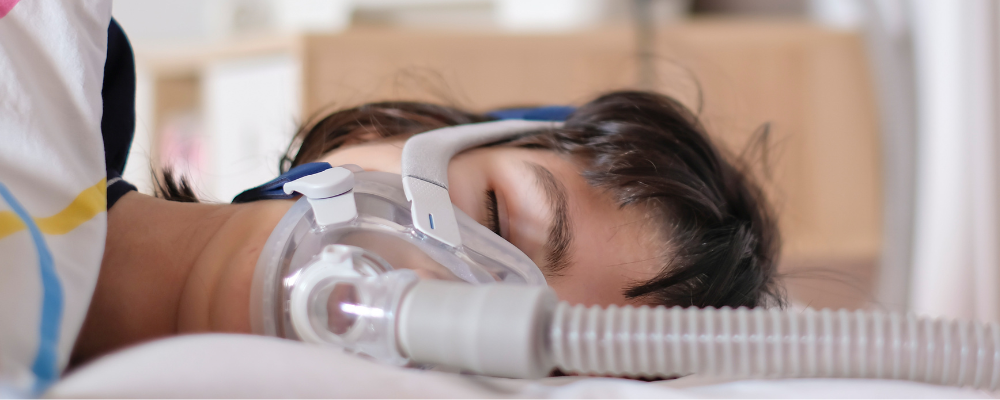
I was diagnosed with obstructive sleep apnea in 2008, long after my initial diagnosis with depression and anxiety. I noticed when I started CPAP treatment that my sleep improved and so did my mood swings. Even with this improvement, I noticed after I drank alcohol, I was much more likely to wake up during the night and, even though I rarely had a hangover, I felt decidedly blue on the mornings after.
We don’t really think of alcohol as a depressant but that is exactly what it does to our body. As explained in one study, “...a typical depressant, alcohol affects the brain in many ways, and it is likely that high doses will cause feelings of sadness (i.e., depression) during intoxication that evolve into feelings of nervousness (i.e., anxiety) during the subsequent hangover and withdrawal.”
It’s such a personal decision, whether to drink alcohol or not. For people with depression and anxiety (and OSA especially,) I think it’s well worth a trial period without drinking alcohol to take note of how you feel. I lost a dear friend to suicide. …it still feels unreal to write that sentence. If anything can be taken from such a loss, it is the need to raise awareness about the support and treatment available for people dealing with sleep apnea and depression.
In my case, I started with a primary care physician and that worked well to manage my anxiety and depression. However, in extreme and emergency situations, there is so much help available. Advocate for your psychiatric care, your sleep care, and everything in between! It can save your life.
If you struggle with suicidal thoughts, please call the Suicide and Crisis Lifeline; anyone can access it free, 24/7 by dialing 988. Confidential treatment for both English and Spanish speakers are available now.
References
“In Brief: Cognitive Behavioral Therapy (CBT).” InformedHealth.Org [Internet]., U.S. National Library of Medicine, 2 June 2022, www.ncbi.nlm.nih.gov/books/NBK279297/.
Sweetman A, Lack L, Lambert S, Gradisar M, Harris J. Does comorbid obstructive sleep apnea impair the effectiveness of cognitive and behavioral therapy for insomnia? Sleep Med. 2017 Nov;39:38-46. doi: 10.1016/j.sleep.2017.09.003. Epub 2017 Sep 22. PMID: 29157586.
Chung TC, Chung CH, Peng HJ, Tsao CH, Chien WC, Sun HF. An analysis of whether sleep disorder will result in postpartum depression. Oncotarget. 2018 May 18;9(38):25304-25314. doi: 10.18632/oncotarget.25219. PMID: 29861873; PMCID: PMC5982747.
“Major Depression.” National Institute of Mental Health, U.S. Department of Health and Human Services, July 2023, www.nimh.nih.gov/health/statistics/major-depression.
Noetel M, Sanders T, Gallardo-Gómez D, Taylor P, del Pozo Cruz B, van den Hoek D et al. Effect of exercise for depression: systematic review and network meta-analysis of randomised controlled trials BMJ 2024; 384 :e075847 doi:10.1136/bmj-2023-075847.
Schuckit MA. Alcohol, Anxiety, and Depressive Disorders. Alcohol Health Res World. 1996;20(2):81-85. PMID: 31798156; PMCID: PMC6876499.